Vaccines and Omicron mean Covid now less deadly than flu in England
A combination of high levels of immunity and the reduced severity of the Omicron variant has rendered Covid-19 less lethal than influenza for the vast majority of people in England, according to a Financial Times analysis of official data.
But the speed with which Omicron infects people still pushed the total number of deaths this winter whose underlying cause was a main respiratory disease to 9,641 since the first week of January, 50 per cent higher than in a typical flu season despite lower levels of social mixing, the Office for National Statistics figures revealed.
The high degree of immune protection from vaccination and previous infection among England’s population formed the basis of the government’s decisions to end legally-enforced self-isolation last month and scale back free testing from April 1 as part of its “living with Covid” plan.
However, experts said a recent uptick in hospitalisations — possibly driven by decreased behavioural caution after the dropping of restrictions or protection from the booster waning for older age groups — highlighted the risk of the government’s strategy.
“Is Omicron the same as flu? No. But the vaccines have made the risks to the individual very similar,” said Dr Raghib Ali, senior clinical research associate in epidemiology at Cambridge university, who added that this made a “large spike” in hospitalisations or deaths “unlikely” while Omicron remained the dominant strain.
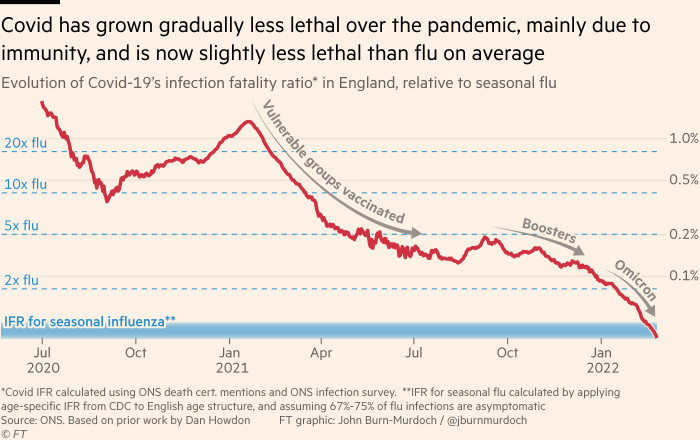
The proportion of people infected with Covid in England who go on to die has dipped below that of seasonal flu, which has an infection fatality rate of 0.04 per cent, for the first time during the pandemic, according to the FT calculations.
Covid’s infection fatality rate fell more than 10-fold from just over 1 per cent in January 2021 to 0.1 per cent in July as the UK’s vaccination campaign was rolled out, and the emergence of Omicron brought about a further three-fold reduction.
For every 100,000 Omicron infections, 35 will result in death, while the equivalent number of flu infections will lead to 40 fatalities, the data showed. Even among the over-80s, where about one-in-200 Omicron infections still results in death, this figure is now lower than the equivalent for flu.
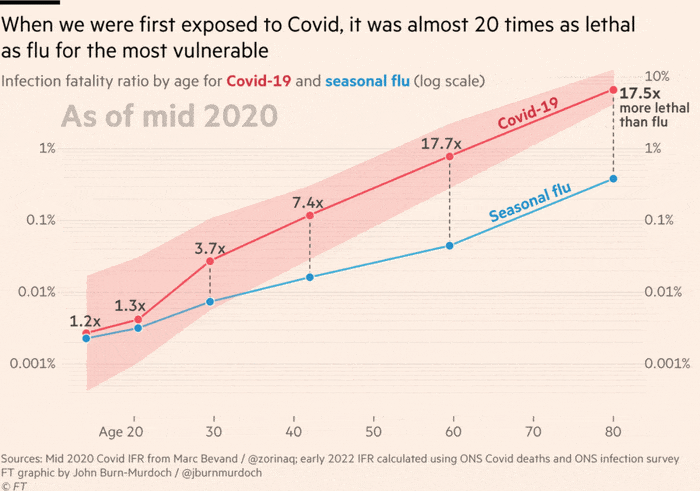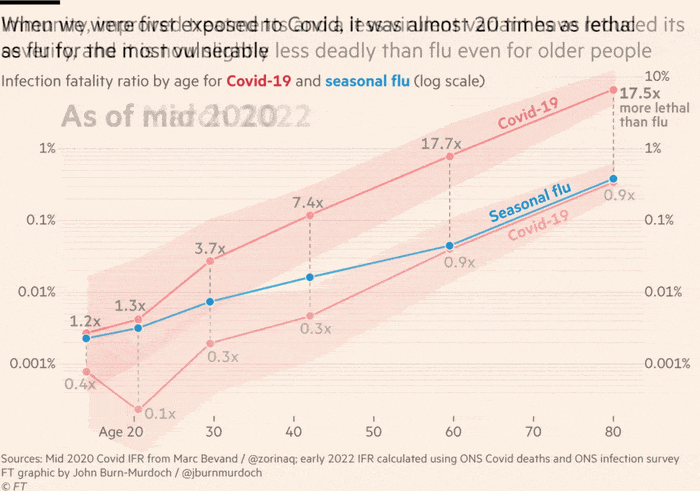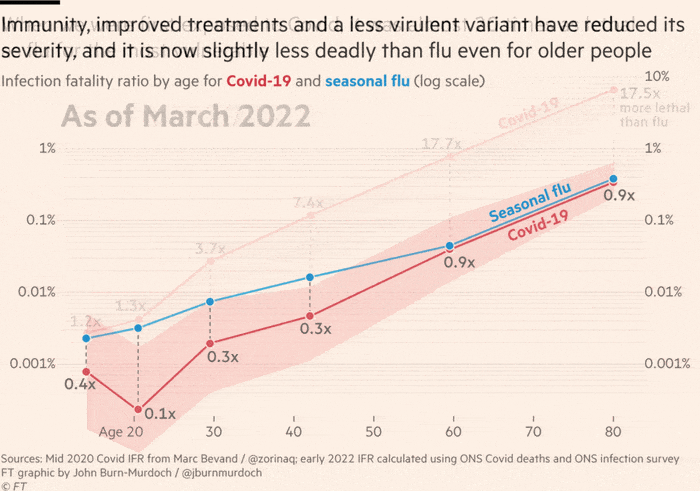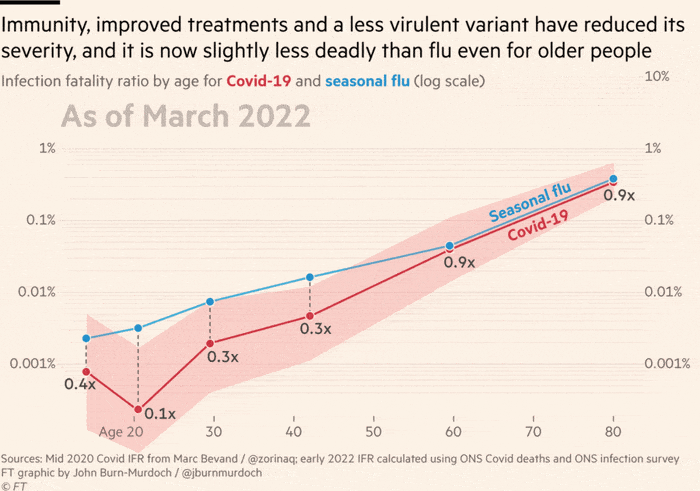
Peter Openshaw, professor of experimental medicine at Imperial College London, said the government’s strategy of treating Covid similarly to flu by relying on public health messaging and targeted testing, instead of bigger interventions, was “risky” but so far “had gone according to plan”.
“If our immunity stays high, the infection fatality rate will stay low,” said Openshaw. But he added that, if waning immunity or a new variant cause problems, “we now have delays built into the system”. “Winding testing down means it will take time to wind it back up,” he added.
Downing Street said on Wednesday: “We still continue to see the effectiveness of vaccinations, and Omicron seems to be more mild for most people.”
After falling for the past two months since the peak of the Omicron wave, Covid-related hospitalisations are on the rise again across the UK. There were 8,153 admissions recorded in England in the week to March 7, up 21 per cent from the week before.

However, more than two-fifths of Covid patients in England’s hospitals are being treated primarily for something else, having incidentally tested positive upon admission.
Unvaccinated people accounted for 15 per cent of adult Covid admissions across England between late January and late February, according to UK Health Security Agency data, despite making up just 9 per cent of the adult population at the start of the period.
Christina Pagel, professor of operational research at University College London and a member of the Independent Sage group of scientific experts, said Omicron’s rapid transmissibility meant “the threat of Covid could still not be equated to flu”. This was especially the case because the BA.2 sub-variant, which is about 30 per cent more infectious than the original Omicron, was dominant in the UK, added Pagel.
Pagel attributed the recent rise in hospitalisations to a mix of waning protection from the vaccines, the spread of BA.2 and the end of most Covid measures giving the virus more chance to infect people and cause severe illness. “I would be really surprised if we have a massive new wave. I wouldn’t be surprised if we end up having what we had with Delta where we get stuck at a high plateau for months and months on end,” she predicted.
Despite vaccination blunting Omicron’s lethality, its fast-spreading nature meant the total number of deaths whose underlying cause was either Covid, flu or pneumonia has still been 50 per cent higher since Omicron took hold in early December than over the same period during a typical flu season. The total respiratory disease fatalities were also 30 per cent higher than even during historically bad flu seasons, such as 2014-15 and 2017-18.

This represents a steep reduction compared to the previous winter’s Alpha variant wave, when there were about seven times as many deaths caused by any of the three respiratory infections, but nonetheless demonstrates that Covid is still adding to the winter disease burden.
However, Cambridge university’s Ali said that now that the risk of Covid and flu were “in the same ballpark” it was “reasonable” for the government to “strike the right balance between preserving people’s freedoms and protecting those who are most vulnerable”.
Prof Julian Hiscox, chair of infection and global health at Liverpool university, cautioned against “complacency” over the reduced threat from Covid, adding that the offer of an additional spring booster should be widened from just over-75s and immunosuppressed people to all over-50s.
“We want to avoid dithering with the extra booster now and then getting caught on the back foot,” said Hiscox, who warned that “all of this could be academic if a new variant comes along”.