US doctors fear patients at risk as cost cuts follow private equity deals
Kevin Robinson, an emergency doctor at a large US hospital, was struggling to fit a breathing tube for a patient when another in an adjacent room developed an abnormal heartbeat.
In many hospitals of equivalent size, Robinson could have called on a doctor of similar experience to supervise the second patient. But here he was alone. For 20 minutes he left a third-year postgraduate student to try — and fail — to stabilise the arrhythmia while he focused on the first patient.
Robinson does not work for the hospital. Instead he is among the hundreds of thousands of emergency doctors employed by a private-equity owned physician staffing group.
Like many of his colleagues, Robinson — whose name has been changed — believes his employer has cut costs so much that conditions are dangerous.
“Clearly this was a patient who would have benefited from supervision by an attending physician,” he said of the person with the heartbeat problem. “For a place with that volume and acuity [medical urgency], it is just not safe not to have multiple attendings supervising the residents and physician assistants.”
Private equity groups have poured money into US healthcare in recent years, as they see opportunity in an ageing society that spends more than ever on staying healthy. According to a report by Richard Scheffler at the University of California, Berkeley, and Laura Alexander at the American Antitrust Institute, annual private equity healthcare deals soared from an estimated $42bn in 2010 to $120bn in 2019, before dipping to $96bn in 2020.
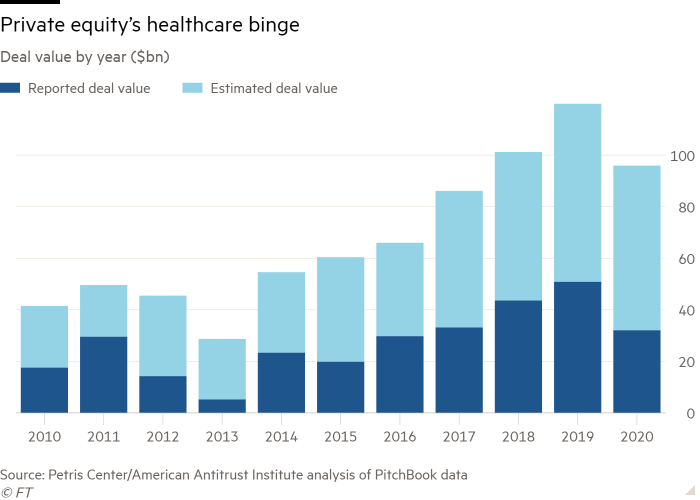
In emergency care, groups such as KKR and Blackstone have bought up physician staffing companies that hire doctors and deploy them at multiple hospitals. The companies contracts and billing and take a share of the insurance or patient payment, which one doctor told the Financial Times can be as high as 50 per cent.
Staffing companies say they are able to offer hospitals greater flexibility over personnel levels on any given day.
But many doctors say that since private equity groups took over several staffing companies in a consolidation wave around five years ago, the companies have been cutting costs by reducing personnel and pay.
The cost cuts have been particularly sharp during the pandemic — even while their subsidiaries have taken tens of millions of dollars’ worth of federal support — in part because of pending legislation that will limit how much companies can charge patients.
The federal No Surprises Act, which comes into force on January 1, will cap the amount that providers can charge for treatments that patients did not choose but for which they are not insured — a practice known as “surprise billing”.
“Private equity companies have been putting the squeeze on doctors with reduced hours and staffing,” said Robert McNamara, head of the emergency medicine department at Temple University Hospital in Philadelphia. “There are fewer doctors on shift, fewer hours, pay cuts and benefit losses. All of this affects the safety of the patient.”
The situation has also sparked concern on Capitol Hill. Elizabeth Warren, the Democratic senator from Massachusetts, said in a statement to the Financial Times: “When private equity firms buy up nursing homes and other healthcare providers, cost-cutting runs rampant, leaving healthcare workers to struggle through staff and supply shortages that endanger patients’ lives.”
Two companies dominate the emergency physician contracting industry: Envision Healthcare, which is owned by KKR, and TeamHealth, which is owned by Blackstone.
Earlier this year Envision put its doctors on a new salary plan, which doctors told the Financial Times would result in roughly 15 per cent lower pay. The new system also linked pay directly to physicians’ ability to bill patients. Doctors said this acts as an incentive to conduct examinations and treatments as quickly as possible.
Envision has also trimmed doctors’ hours and is making increasing use of highly qualified nurses to do some of the work of physicians for about a quarter of the cost, doctors said.
At the same time, an analysis by Bloomberg found that its affiliates claimed at least $60m in government loans meant to support cash-strapped healthcare groups during the pandemic. TeamHealth has also reportedly cut staff hours and asked anaesthetists to go on furlough, while claiming a reported $105m in government assistance.
TeamHealth did not respond to requests to comment before this article was first published. After publication on Thursday, the company provided a statement to the Financial Times.
“Like virtually all providers we had to adjust staffing levels given substantial declines in visits — but we kept those levels substantially above anticipated volumes during the pandemic despite the significant financial cost,” TeamHealth said. “Our clinicians continue to do heroic work for their patients and we are committed to supporting them with the resources they need to provide high-quality care in the face of an ongoing global pandemic.”
Envision said it was “focused on delivering safe, high-quality care that puts the patient first”.
“We tailor our care teams — physicians and advanced practice providers — and models to fit the unique needs of communities, based on several factors, including geographic location and patient population, demand and acuity levels,” Envision said.
Some doctors are alarmed at the situation, however, and are pushing the American College of Emergency Physicians to conduct more research into patient outcomes at hospitals staffed by private equity-run groups.
“There is a workforce crisis in emergency medicine,” said Mitchell Li, a doctor who recently established Take Medicine Back, a group campaigning against corporate ownership of US healthcare. “Private equity groups are slashing costs and making conditions worse for doctors and patients. It is completely unsafe.”
A study earlier this year by the National Bureau of Economic Research found that a patient who goes to a private equity-owned nursing home was 1.7 percentage points more likely to die within the next 90 days than one who went to another facility.
No equivalent study has been done for emergency rooms, though waiting times in many parts of the country are rising rapidly.