Johnson’s new vaccine target sets stern test for GPs and jab centres
An ambitious new target to fully vaccinate two-thirds of England’s adult population by July 19 will test staff on the frontline of the country’s vaccination rollout who have warned of supply shortages and a growing struggle to combine the programme with clearing a huge backlog for non-coronavirus related treatment.
The central role of vaccines in limiting the impact of the third wave now under way in the UK was emphasised on Monday when new data from Public Health England suggested the link between infections and hospital admissions — ironclad in the first two waves — has been substantially weakened. Two shots are highly effective at preventing admission to hospital with the Delta variant now dominant in the UK, the data showed.
The impact of inoculation was borne out by FT analysis that showed people aged 65 and above now make up just 27 per cent of hospital admissions in England, their lowest share since the beginning of the pandemic, and far below the record high of 73 per cent in May 2020.

Within this group, over-85s are now just 8 per cent of admissions, down from a peak of 29 per cent. Despite this marked progress, the most recent data suggest a possible uptick in admissions of people aged 55 to 64, a sign that the virus is finding gaps in vaccine coverage. 850,000 people in this age group are yet to have a single dose, and 1.4m have only one dose.
The central estimates for a July 19 unlocking produced by the government’s scientific advisers still suggest peaks of more than 1,000 hospital admissions and 100 deaths per day in August and September.
In a press conference on Monday evening to announce a delay to plans to fully lift Covid-19 lockdown restrictions scheduled for next week, prime minister Boris Johnson stressed the plan to target all over 40s by reducing the interval between doses to eight weeks to limit the threat posed by the Delta variant.
Modelling by the Sage advisory group also suggested that, given the likely transmission advantage of the Delta variant, more than 80 per cent of the population — adults and children — would need to develop immunity through vaccination or natural infection to achieve “herd immunity”.
Separately, a nationwide study in Scotland published in The Lancet found cases of the Delta variant were nearly twice as likely to require hospital treatment compared to people who tested positive for the previously dominant Alpha strain of the virus.
However the two main vaccines on offer in the UK — BioNTech/Pfizer and Oxford/AstraZeneca — offered “very, very substantive” protection, according to the researchers behind the study.
As ministers now look to ramp up vaccinations, staff at the forefront of the UK’s vaccination drive — considered one of the world’s most effective — are struggling to overcome a range of obstacles, from hesitancy to supply shortages.
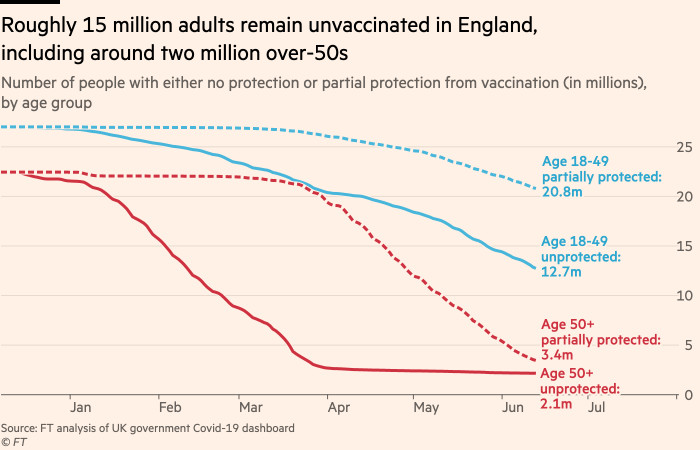
A total of 14.8m adults in England are yet to receive a single vaccine dose, according to the latest data from Public Health England. This includes 2.1m people aged 50 or over, a figure that remains stubbornly high, falling by only one per cent in the past week.
According to government data for June 13, 25.4m adults in England have received two doses of a coronavirus vaccine. To reach two-thirds of England’s adult population would mean delivering over 3m jabs between now and July 19, according to FT estimates. The current vaccine delivery rate averaged 239,000 in England over the past seven days but this also included administering first doses to people.
Ruth Rankine of the NHS Confederation, who represents networks of GPs who have run the bulk of the vaccination programme, said there was still significant work to do to ensure all eligible Britons were vaccinated.
In some cases GPs were refocusing “their time and capacity on dealing with their backlog particularly where there are mass sites nearby who can pick up the vaccination work”, she said. Primary care workload was “increasingly more complex”, with the need to manage symptoms of patients on hospital waiting lists as well as those with mental health problems. “We have also heard reports from our members about shortages of the Pfizer vaccine which is needed for the under-40s cohorts”, Rankine added.
Greg Fell, public health director for Sheffield, said an unresolved issue was how to direct supplies to the areas with lowest uptake. Noting that 75 per cent of vaccinations so far had been carried out in GP-run centres, he added: “Their ability to keep going at the current run rate, never mind accelerating it, requires a lot of careful thought and attention, because the last thing anyone wants to do is to break primary care in the process.”
Professor Martin Marshall, chair of the Royal College of GPs, echoed concerns about GPs’ ability to continue to play such a large part in the vaccination process given the pressure they are under to restore normal services to patients.
Anecdotal evidence suggested that a growing number of GPs were giving up their vaccination responsibilities. “They feel they need to go back to concentrating on business as usual and then come back in the autumn when there will be a need to give booster shots,” he added.
Marshall also suggested there was an continuing struggle to reach people who had been resistant to getting the vaccine. “Overall the vaccination rate is incredibly high, much higher than anyone expected it would be and much higher in the UK than other countries.” But he compared the 80 per cent of older people nationally who had been vaccinated, to around 50 per cent in his own area of east London where there was a large ethnic minority population, a group whose members had proved more reluctant to get the vaccine.
Through moves such as holding vaccination clinics in religious establishments and sending buses into communities, they were persuading people to get the jab, he added. “It’s slow and it’s hard work but it is working,” Marshall said.