Covid risks deepening NHS ‘permanent winter’
England’s NHS is not increasing the number of patients it treats quickly enough to reduce a massive backlog of non-urgent care as it braces for the impact of the Omicron variant, according to Financial Times research that shows a service beset by workforce shortages and constraints imposed by Covid-19.
Boris Johnson’s announcement on Sunday that all over-18s will be offered a booster jab by the end of December has trained a harsh spotlight on the NHS’s ability to cope with the multiple demands it now faces. Our research suggests that even before it confronted this new obligation, the health service was entering winter in its worst ever shape.
The arrival of Omicron has potentially exacerbated this trend. In the first of its annual audits of the NHS, the FT in 2017 identified a health service living through a state of “permanent winter” with intense strains on the taxpayer-funded system barely letting up even in months that would once have given it a chance to catch its breath.
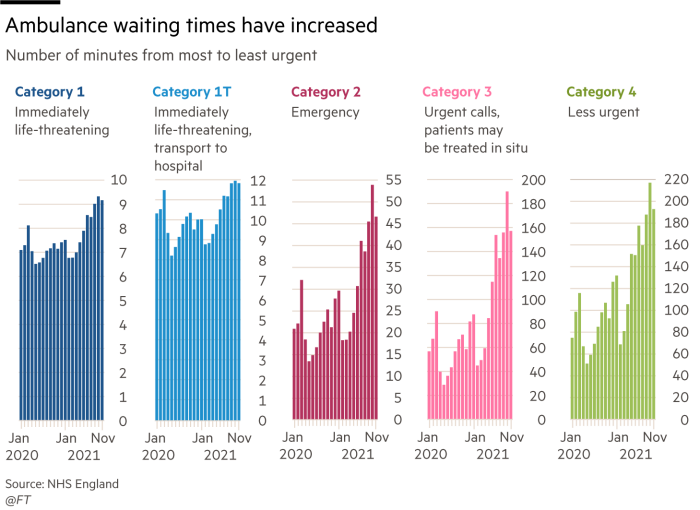
Five years on, after having suffered the then-unimaginable shock of Covid-19, waiting lists are more than 2m higher. Suspected cancer sufferers are facing longer waits, callout times for ambulances are rising sharply and the requirement that most people should wait no more than four hours to be treated in emergency departments is being missed by record margins.
Matthew Taylor, chief executive of the NHS Confederation, which represents health organisations across the UK, said: “The NHS and care system faces an emergency and that emergency is going to continue until the end of winter at least.”
He suggested that the cause lay partly in spending cuts instituted by the 2010 coalition government. “Part of the reason we are where we are is because of the impact of the austerity decade,” he said, adding that it was “the lowest decade of growth in health service expenditure since the NHS was created”.
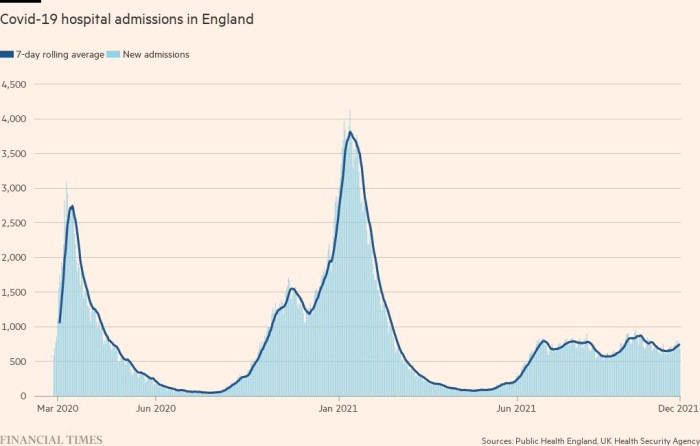
So far there are few signs that the NHS will be overwhelmed by Covid alone. In England, daily hospital admissions for the disease peaked at 4,134 in January 2021. The most recent data showed that the equivalent figure is currently 696.
However, the impact of the virus on the health system has been profound. Infection control measures have reduced the number of beds in use and absorbed the energies of key staff, including anaesthetists, who would otherwise have been free to treat patients on waiting lists.
Sajid Javid, health and social care secretary, acknowledged on Monday that operations such as hip and knee replacements would be postponed until the new year as staff focused on the turbocharged Covid vaccine booster campaign.
However, what emerges most strongly from the FT’s analysis of official data is that even before Omicron changed the calculus, the health service had been unable to pick up the pace sufficiently to prevent waiting lists spiralling even higher.
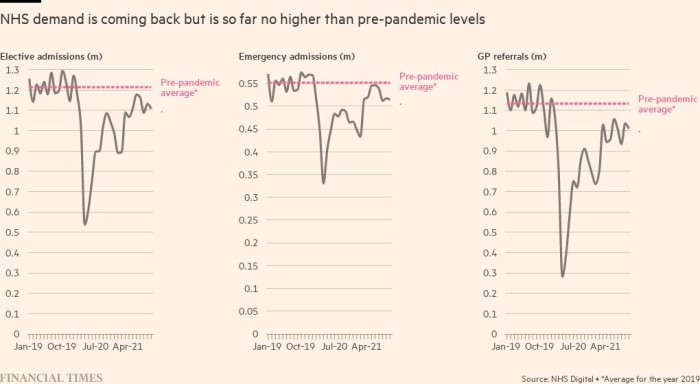
While referrals and admissions have been approaching pre-pandemic levels — evidence of a system making up lost ground — only by treating substantially more people each month than before the coronavirus crisis can the NHS reduce the ever-expanding queue for care.
The idea that this could be achieved in the short term may never have been realistic, suggested Richard Murray, chief executive of the King’s Fund. Even before Covid hit, every indicator was flashing red, with waiting lists lengthening and treatment targets missed.
“If the NHS couldn’t turn things around in 2019, what do we think’s changed so much that it could be done in 2021? I think there was always a little bit of magical thinking in suggesting the NHS would be able to ramp up activity well above pre-Covid levels,” he said.
The growing backlog presents clear political risks for ministers, who are anxious to demonstrate that the service is improving as they prepare to raise national insurance contributions to help fund a further £30bn of funding for the health service.
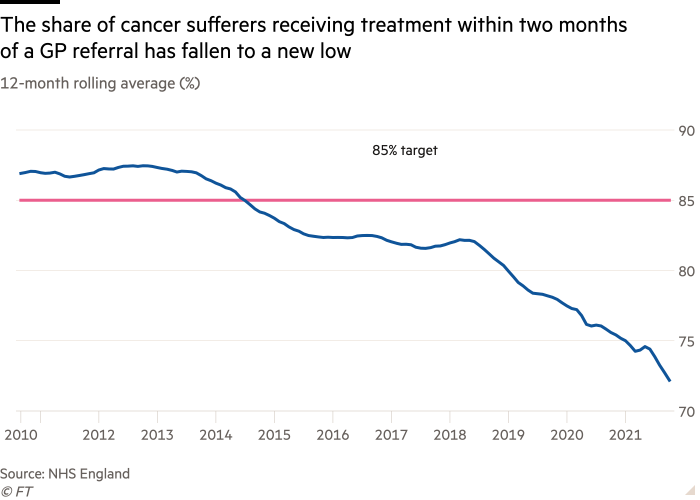
John Appleby, chief economist at the Nuffield Trust, said a particular concern was evidence that the number of people waiting more than two weeks to see a cancer specialist, and two months to start treatment after a referral, were on the rise. “They are the urgent of the urgent and you can see how way above target they are and they’re going up,” Appleby said.
The lengthening queues come despite the fact that cancer is one area where the NHS has managed to deliver more appointments than before the pandemic “but it’s still not keeping up with the flow of referrals from GPs”, Appleby noted.
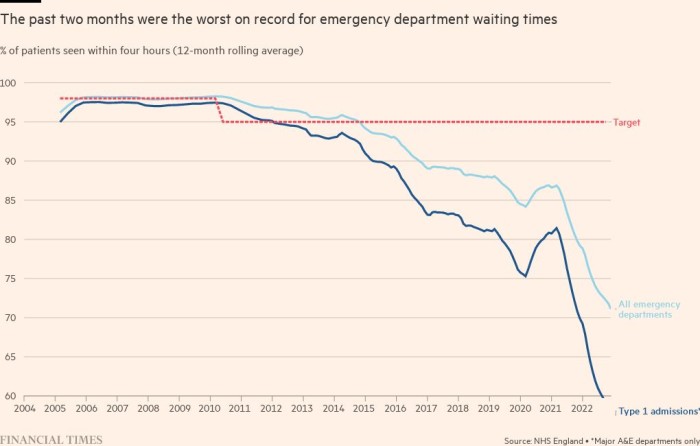
Strains on the wider system tend to culminate in hospital emergency departments. Dr Adrian Boyle, a frontline A&E specialist who is vice-president of the Royal College of Emergency Medicine, said the service had just recorded its worst-ever performance against a target that at least 95 per cent of A&E patients should be treated within four hours. Almost four out of 10 now wait longer — despite a fall of about 50,000 in the number coming to A&E in November this year compared with two years ago.
He highlighted bed shortages as a key reason for the bottlenecks, estimating that 10-20 per cent of hospital beds were taken up by people who did not need to be there “because of a lack of social and community services, basically”. In addition, about 7 per cent of the national bed stock was being taken up by Covid patients, he added.
The resulting delays in admitting patients brought in by ambulance in turn delayed crews reaching other patients who needed emergency help. “We are hearing increasingly about people who are dying because an ambulance doesn’t get to them in time,” Boyle added.
The backdrop to these pressures is an acute workforce crisis, with about 100,000 vacancies across the health service. Vacancies for medical practitioners have risen by 15 per cent in the past year, while for nurses they are up 7 per cent.
Murray suggested that this reflected the UK’s lean approach to public services, where the priority is avoiding unnecessary expenditure. “If you look at many European countries, they overtrain, they are very, very anxious about running into a workforce shortage,” he said. “I think this country is the other way around. We have tolerated repeated workforce shortages,” he added.
The key question for ministers and health leaders is whether the NHS can find a way of treating many more patients in the years ahead by raising its performance above the trend rate of recent years.
A so-called “elective recovery” plan, due to be published around the start of the month but delayed because of Omicron, is expected to suggest a rethink in the way some services are delivered to make better use of resources. This includes reducing outpatient appointments through a system of “Patient Initiated Follow Up”, using surgical hubs to deliver routine operations and incentivising hospitals to carry out more work.
But Murray cautioned that staff shortages were likely to undermine such initiatives: “It just keeps coming back again and again and again to the workforce issue,” he said.
Taylor suggested that the way the NHS cared for patients over the next decade could be transformed by technological advances and better collaboration between different parts of the health and social care system to improve the health of the population.
But he warned that it was vital that the government and NHS leaders were straight with the public about how long it would take to clear the backlogs. “One of the things that we’ve seen during Covid, unfortunately, has been a tendency to overpromise in terms of test and trace or whatever it might be . . . I think the public are perfectly able to hear those two messages: realism about the challenges now but excitement about where we can get to in the future.”
NHS England said staff were “continuing to make progress on elective activity”, with almost 150,000 more people starting treatment in October compared to the same month last year.
At the end of October, patients were waiting an average of 12 weeks to begin treatment, compared to a high of 19.6 weeks in July last year, it added.