America’s Covid testing system buckles under weight of Omicron surge
Almost a year since President Joe Biden took office pledging to bring the pandemic under control, the Omicron variant threatens to overwhelm the country’s Covid-19 testing system, causing chaos for people seeking to travel, return to work or school, or visit elderly parents.
The surge in infections has led to an explosion in demand for rapid antigen tests and more accurate PCR laboratory tests, with many retailers selling out of kits and labs struggling to deliver results on time.
In some parts of the country people are queueing for hours in freezing conditions to be tested, increasing the risk of spreading the virus. Others have been forced to cancel family gatherings, flights or postpone children’s return to school because of problems with testing, prompting growing frustration at the government’s pandemic response.
Dr Zeke Emanuel, a professor of healthcare management at the University of Pennsylvania and a former Covid adviser to Biden, said: “Everyone thought the vaccines were going to solve everything, which meant the administration took its eye off the ball when it came to testing.”
Calculations by Mara Aspinall, a professor of biomedical diagnostics at Arizona State University, suggest the US currently has a capacity of 260m at-home tests per month, though that is likely to double by March.
Many of those are being used by large institutions such as schools and workplaces, making it difficult to find test kits at pharmacies or other retailers.
The White House is finalising contracts for an additional 500m at-home tests — enough for two for every adult — though it has not yet said how long those contracts will take to deliver.
The US is not the only country experiencing a shortage of at-home tests as cases explode, fuelled by the highly transmissible Omicron strain. The UK, Australia and several parts of Europe are also struggling to provide kits for all those who want them.
A White House official said: “The reality is there is unprecedented demand across the globe because of Omicron, which is stretching testing capacity for many countries.”
But the situation in the US is a source of particular frustration for many. Tests were in such plentiful supply over the summer that Abbott, the largest provider of rapid tests, laid off hundreds of workers and disposed of millions of components at that time.
That decision came amid falling cases and changed guidance from the US Centers for Disease Control and Prevention exempting people who had been vaccinated from testing when exposed to the disease.
Aspinall said: “There was an optimism around the vaccine, which was well founded, but it led to a response from the administration which was not flexible enough to deal with a rapidly changing virus.”
Now US hospitals are appealing to the public with only minor symptoms to stop flooding emergency rooms in search of testing because of the nationwide shortfall. And some health experts are warning that testing delays propagate the virus and could blunt new antiviral treatments for Covid which need to be administered within days of infection.
“It kind of shook my faith in the testing process,” said Mary Ellen Carafice, who works at a school in Brooklyn and cancelled plans to visit her mother over Christmas because of delays in receiving test results.
The week before Christmas she waited four days to receive results from a PCR test conducted by LabQ Diagnostics — a company warned by New York authorities that it may be in breach of “false advertising” laws for failing to deliver on its promise of providing results within 48 hours.
The delays forced Carafice, who had Covid-19 symptoms, and her partner to book a further PCR test with an alternative provider and join the race to locate and buy rapid antigen tests. She later tested negative but her partner received a false positive result and Carafice was forced to eat Christmas dinner with her elderly mother over a zoom call.
LabQ did not reply to a request for comment but a recorded telephone message said that, this week, results could now take up to five days to deliver. The waiting time to speak to a LabQ operator was more than an hour.
Safety concerns linked to inadequate testing prompted the closure of public schools in Chicago this week following a vote by teachers’ unions. Some US states have begun restricting access to publicly supplied rapid antigen tests to vulnerable age groups because of tight supply. And the CDC issued controversial guidance that does not require a person with a Covid infection to test negative in order to leave isolation after five days — a move that experts say is prompted by a shortage of tests and risks confusing the public.
“I only wish the US had followed the UK and Germany, where from very early in the pandemic their governments supported ramping up the testing supply chain and provided messaging that rapid testing was a valued component of the pandemic response,” said Carri Chan, director of Columbia Business School’s healthcare programme.
Inconsistent messaging from the US administration on the value of rapid testing had caused the private sector to hesitate about increasing production, leaving the nation exposed when global demand soared because of Omicron, she added.
Dr Henry Walke, director of the CDC’s Division of Preparedness and Emerging Infections, warned on Friday against using self-administered antigen tests as a way to decide whether or not to return to work.
“A negative antigen test doesn’t necessarily mean that there’s an absence of a virus,” he said.
Abbott and other makers of rapid antigen tests are now scaling up manufacturing capacity again but are battling labour shortages, shipping delays and competition for components amid the global surge in demand for tests.
“It has taken a year-and-a-half for the US to embrace the important role of rapid testing. Overseas, that was not the case,” said an Abbott spokesman.
“We always said that testing would be needed, together with vaccines, to keep people in the office, kids in school, events from being cancelled, and congregate care facilities safer.”
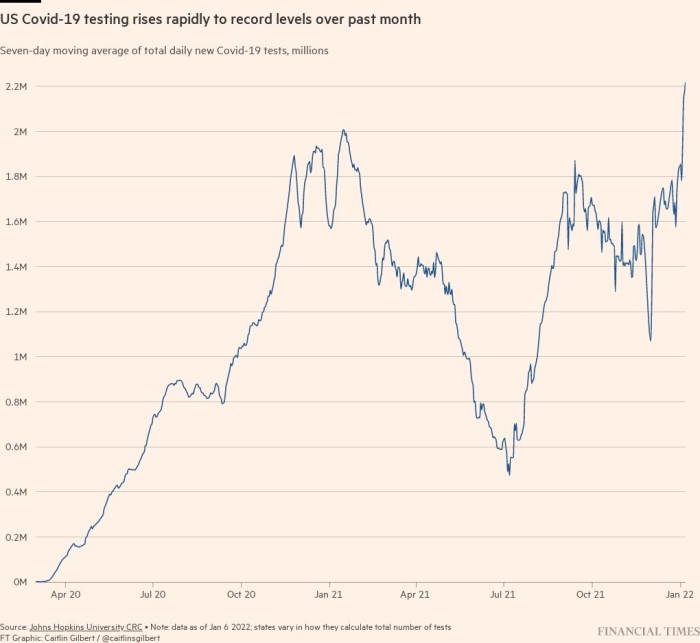
The largest providers of laboratory tests in the US are also struggling to keep up with demand. Covid testing has increased by 130 per cent to a record 2.2m tests each day since the Omicron variant was identified in late November, according to data from Johns Hopkins University. PCR and other molecular testing alone has increased by 40 per cent to 1.7m tests each day. Antigen testing is probably undercounted with many states not reporting or collecting that data amid widespread at-home test use.
Quest Diagnostics said average turnround times for results had blown out from within 24 hours to two to three days because of the Omicron surge. Other industry participants, who did not want to be named, said some labs were facing labour shortages due to staff absenteeism linked to infections.
Elliot Glotfelty, a student in Baltimore, who queued for four hours on Wednesday for a PCR test, told the FT he feared he could catch Covid while waiting in line. By Friday evening he still had not received his result.
“Waiting long periods kind of defeats the purpose of testing,” said Glotfelty, who was tested after experiencing symptoms. “My brother and sister teach in a city school and they sometimes don’t get results for over a week which kind of defeats the purpose of tracing.”