Will ‘open-source’ vaccines narrow the inequality gap exposed by Covid?
Soumya Swaminathan’s “aha moment” came in February 2021. Covid-19 had been ravaging the world for 12 months and vaccines had only just begun a slow trickle into richer countries, but were nowhere to be seen in poorer ones.
Swaminathan, the World Health Organization’s chief scientist, had been on a call with Tedros Adhanom Ghebreyesus, the health body’s director-general, French president Emmanuel Macron and others, to discuss access to vaccines. “Macron said something about [a] lack of manufacturing capacity [for Covid vaccines] and that all the manufacturing is concentrated in a few regions,” Swaminathan says. “That planted a seed in my mind.”
A little over a year later, that seed has morphed into a potential high-tech revolution in mRNA vaccines that could transform access to all sorts of medicines, not just for current health emergencies, such as Covid, but also the next one — whatever it might be.
Spearheaded by the WHO, the setting for this radical overhaul is a series of nondescript warehouses on a Cape Town industrial estate, next to a factory-sale bed shop. It is there, at the headquarters of Afrigen Biologics and Vaccines, a South African start-up, that late one night in January a scientist walked into the office of Petro Terblanche, the company’s managing director, and announced a breakthrough. Afrigen, a member of a hub — of scientists and pharmaceutical companies — created to develop mRNA vaccines, had successfully formulated a replica of Moderna’s Covid vaccine. It used publicly available information and relied on the drugmaker’s commitment not to enforce its intellectual property rights during he pandemic. The first human trials of the copycat drug could start in November.
A year ago, “there was a sense that this was too difficult, that scientists in Africa could not make this,” Terblanche says. But Afrigen’s team worked up a detailed plan even before going into the lab, she adds. “They have run this in a very short period of time.”

Over the past two years, global health authorities have consistently warned of iniquitous access to tools — from testing to drugs and vaccines — to help counter the pandemic. High-income nations such as the UK, the US and those in Europe began their vaccine rollouts in December 2020, having reached substantial proportions of vulnerable groups by February 2021.
The first shipment of vaccines — 600,000 doses of the Oxford/AstraZeneca version — delivered by Covax, the WHO-backed access programme, only arrived in the Ghanaian capital, Accra, in late February 2021. Since then mRNA manufacturers, such as BioNTech/Pfizer and Moderna, have booked record-breaking revenues and become key players in business and geopolitics.
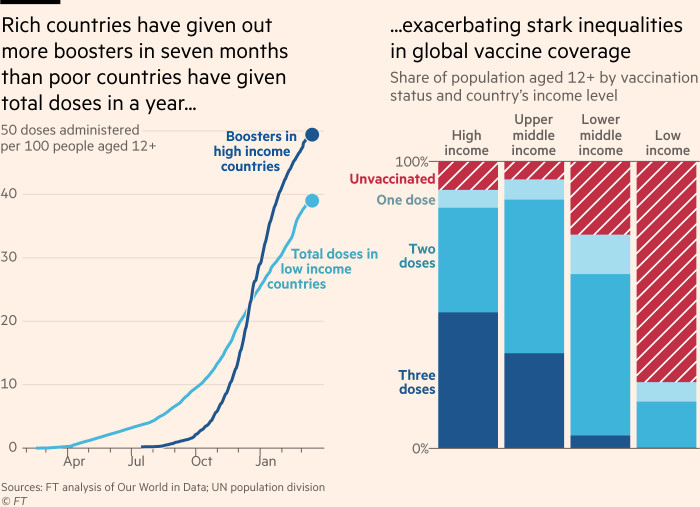
Yet, more than three-quarters of people in low-income countries aged 12 and over have still to receive a single dose, compared with 10 per cent in high-income countries, according to Our World in Data, the research group.
The Cape Town initiative is part of a new push by global health authorities, academics and philanthropists to address that and promote alternatives to “Big Pharma’s” business model, which relies on legally enforceable patent protections to raise investment to fund new drugs. The chronic lack of access to vaccines in the developing world has emboldened some researchers to embrace the concept of “open-source pharma” — an idea modelled on the free software movement, which encourages collaboration and sharing to improve code.

Matthew Todd, chair of drug discovery at University College London and one of the founders of the open-source pharmaceuticals initiative, says the pandemic has driven global collaboration on developing vaccines and antiviral treatments, which could have a lasting impact on the industry. “The idea of sharing everything you’re doing and developing a medicine that’s freely available with liberal freedoms associated with it is really quite a new thing,” he says.
Industry experts vociferously oppose weakening protections for intellectual property, which they say are critical to incentivising companies to take risks. “We deployed $2bn before we knew whether we could successfully develop a vaccine because we understood what was at stake,” Albert Bourla, Pfizer chief executive said in an open letter published last year. “I worry that waiving of patent protection will disincentivise anyone else from taking a big risk.”
For months, the battle for access was centred on intellectual property rights. But the so-called Trips waiver — proposed by India and South Africa in 2020 — which would allow for flexibility in patents for the manufacture of vaccines, is still being discussed at the World Trade Organization. The hub, in contrast, aims to make the technology accessible to poorer nations and also train qualified staff to produce vaccines locally without breaking any intellectual property rules.
“There was a lot of scepticism from a lot of people, ‘It’ll be a failure. WHO can’t do it’,” says Swaminathan, who is still cautious: “I want to be very realistic here. The fact we set up this programme is a long way [from] achieving success.”

Stéphane Bancel, the chief executive of Moderna, has his own reservations. “We’ve never helped them develop it or make it. We have never certified their quality control. They are claiming it’s a copy of Moderna’s product. I don’t know,” he told the Financial Times in November. “It is like when somebody makes a copy of a Louis Vuitton bag. Does it look like a Louis Vuitton bag? Does it last like a Louis Vuitton bag? I don’t know.”
In response to criticism from social justice advocates that Moderna risked harming the WHO-backed project, the company last week said it would not enforce its Covid vaccine patents against the hub or other manufacturers seeking to make jabs solely for 92 low- and middle-income nations.
Closing the vaccination gap
Martin Friede, the co-ordinator of the WHO’s initiative for vaccine research, says the new scheme is drawing on experience from a previous hub, set up to spark production of pandemic influenza vaccines.
“This was a copy [and] paste” of a 2006 plan that came about after an H5N1 scare the previous year, with several hundred cases in the Far East with high mortality, he says. Even then, says Friede, poorer countries, facing the brunt of the disease, risked being left out by richer ones. “These countries [Indonesia, Thailand and others] were saying: ‘This is not fair. We’re the ones facing the virus. You’ve got the vaccines and we know there’s not enough vaccine to go around’.”
“When we started in 2006, the total production capacity [for pandemic influenza vaccines] in lower- and middle-income countries was zero doses,” says Friede. In 2015, it was 1.3bn, helped by that hub set up in the Netherlands.

He says the mRNA initiative has received at least €40mn from a host of countries including France, Germany, South Africa and others, while the Geneva-based Medicines Patent Pool, a non-profit group that has helped strike low-income country access deals for Covid drugs, assists with legal and licensing aspects of its work.
Marie-Paule Kieny, the director of research at France’s National Institute of Health and Medical Research (Inserm) and a WHO veteran, has been pivotal in creating these hubs, according to Friede and Swaminathan. And she successfully lobbied Macron and his advisers to help bankroll the mRNA version.
The South African hub has a series of “spokes”, or recipients of the technology in Africa and beyond. The theory is that they will harness the technology locally, for Covid or other as-yet-unidentified diseases. The WHO has also established a centre in South Korea to help train the workers needed to produce and manufacture the vaccine. A shortage of such specialists has previously been used to justify the rejection of calls from wealthier countries, such as Italy, to set up domestic mRNA production.
‘The world’s vaccine’
Even if it passes all of its regulatory hurdles, Afrigen’s will not be the first open-source vaccine to go into people’s arms, although it would be the first mRNA one to do so. Some countries, such as Cuba, have invested heavily over the years to create a public and domestic biotech sector to help produce drugs if and when needed.
It now has one of the world’s highest Covid vaccination rates in adults and children above the age of two and has been using protein-based shots, a more traditional type of technology that is easier to make and store.
“[Cuba’s] public patents are free to facilitate tech transfer,” says Fabrizio Chiodo, a scientific researcher at Italy’s national research centre and Cuba’s Finlay institute, “with a royalty to be paid [to the state] on a case-by-case basis”.
In February, a team at the Texas Children’s Hospital Center for Vaccine Development in Houston celebrated the roll out of Corbevax, a patent-free vaccine costing less than $2 a shot, which has been granted emergency use authorisation in India.

Biological E Limited, a Hyderabad vaccine and pharmaceutical company, licensed the technology developed by the Texas vaccine centre at low cost from BCM Ventures, part of Baylor College of Medicine, and has a contract with the Indian government to deliver 300mn doses. There are hopes the jab can also be rolled out in Bangladesh and Indonesia, where regulatory approvals are being sought, and in Africa, where there are plans to set up manufacturing in Botswana.
Unlike the mRNA jabs developed by BioNTech/Pfizer and Moderna, there is no requirement for storage at very low temperatures — a key advantage in administering the vaccine in developing nations. Corbevax provides 90 per cent efficacy against symptomatic infection from the original Wuhan strain of Covid and 80 per cent against Delta, according to two phase-3 clinical trials conducted by Biological E. The results are awaiting peer review.
“In an emergency you want to make sure there are no barriers,” says Maria Elena Bottazzi, one of the principal researchers who developed the Texas vaccine, explaining why they deliberately waived intellectual property rights and chose an old-fashioned protein-based vaccine technology, which is easy to replicate.
“It’s not just a matter of patent deed restrictions. There is the technical knowhow, there is the practice, [people] need help in knowing how to make the vaccine — and that’s what we provide as well,” says Peter Hotez, another researcher on Corbevax, who has been nominated, along with Bottazzi, for the Nobel Peace Prize by local congresswoman Lizzie Fletcher.
The Texas research team failed to secure cash from the US government’s multibillion-dollar Warp Speed programme, which supported the Moderna and Novavax mRNA vaccines. Instead, it raised $7mn in philanthropic donations, including from a Texan vodka maker to fund the project.
Bottazzi says their success in developing and licensing its open-source vaccine could become a model for how to tackle future pandemics.
“It would create this self-sufficiency, a validation that it was made indigenously. People could learn from it and become to a certain degree decolonised by it. They don’t have to wait all the time to receive solutions from high-income countries,” she adds. “We call it ‘the world’s vaccine’ because it can very rapidly be shared and provided to countries through Covax or other mechanisms to tackle global vaccine inequality.”
A cost-effective pandemic insurance
Backers of open-source vaccines say it is difficult to fully assess their potential. But for the WHO’s Swaminathan there is one clear opportunity: “they will get into production in the inter-pandemic period”.
Her hope is that the world can be better prepared to roll out speedy vaccines to all when and if the next pandemic hits. “My dream would be that if there’s an outbreak of a virus next time,” says Swaminathan, “that as soon as the genetic sequence is done and there are these platforms that are ready to go that the tech [can be] shared immediately around the world, then you’re ready and pumping out vaccines . . . It’s not just about producing Covid vaccines and then closing shop.”

Friede argues that building a “relatively small facility” is a cost-effective pandemic insurance. “You can have parts of it ‘mothballed’, kept in a sterile room, and roll it out if and when the next pandemic strikes. You’re going to keep your knowhow warm at non-horrendous costs,” he adds, before conceding that some countries would have to rationalise how the facilities are kept between public health emergencies.
“You keep a skeleton staff operating this at low scale to make sure the knowhow doesn’t leave,” he says.
The vaccines would also need a market — or governments willing to buy doses annually or in advance to make the venture financially viable.
“In between pandemics it’s going to cost a lot of money just to keep the fans running, the filters clean and the lights on. This is going to be a strategic decision made by each country,” Friede says.

Even if the mRNA hub faces some scepticism, and on occasions open resistance from the industry, Inserm’s Kieny says “we’ve never been in a conflicting situation with Moderna”.
The drugmaker, which has pledged not to enforce any patents during the pandemic but reserved the right to do so when it ends, is facing a separate intellectual property case. The biotech company, whose vaccine is its first approved product, is being sued by rivals Arbutus Biopharma and Genevant Sciences over “patent infringement” allegations. Moderna denies the allegations and plans to fight the case in court. It has also been involved in a heated dispute with the National Institutes of Health, which helped research its Covid vaccine, over the invention of a key component of its jab.
Kieny says that in the previous hub, for pandemic influenza, patents were not an issue as they had expired. And patent-free drug development itself is not new: it has been used for the polio vaccine and penicillin.
But the promise of the open-source model is, according to its backers, unprecedented. “A year ago we thought that if only we could get Moderna to give us the tech, the recipe, we would fast-track [vaccine production],” says Afrigen’s Terblanche.
“Today, I am in a way grateful that they didn’t, because a turnkey tech transfer from a company like Moderna or Pfizer, you get a box, you sit in the box, and your freedom sits only in that box. The scientists would have learned to bake,” she says. “Now they have learned to make.”