Pandemic exposes a world of healthcare inequalities
As the world enters its third year of reluctant coexistence with coronavirus, global health systems are straining under the impact of the hyper-infectious Omicron variant. But, even as countries continue to battle the pandemic, their leaders are thinking about ways to shape a society that will be better prepared for the next health emergency.
They are considering not only how to deliver a more agile response to future emerging pathogens but also how to tackle the health inequalities so brutally exposed in the past two years — in the rich world, as well as the global south.
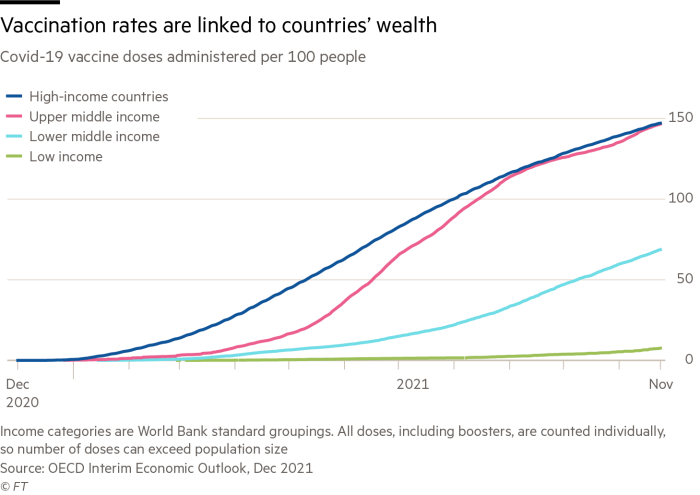
Vaccination remains a yawning divide between the west and the developing world. While just under 60 per cent of the global population has received at least one vaccine dose, the figure for people in low-income countries is only 9.5 per cent, according to research organisation Our World in Data.
The statistics point both to issues of supply and to the need for better infrastructure to administer the shots that have proved so effective at reducing Covid-19 hospitalisations and deaths.
David Heymann, a distinguished fellow in the global health programme at Chatham House, a London-based think-tank, notes that many lower- and middle-income countries, unaccustomed to the mass flu immunisation campaigns carried out in western nations, lack established systems for delivering vaccinations at scale.
“So it’s not just a matter of saying the Covax facility [a procurement scheme set up to give people in poor countries equitable access to vaccines] will give you vaccines, it’s a matter of making sure that countries are ready for those vaccines and are willing to use them,” he says.
African countries, for example, may have a different perspective on the urgency of Covid vaccination than western countries because they have a different overall burden of disease. Heymann says that, during a recent meeting in Ghana, some of Africa’s public health leaders told him that “Covid vaccines are not our priority — we want malaria vaccines, we want vaccines which are for diseases that are causing high mortality in our countries.”
Such concerns are underscored by data that show the collateral damage inflicted on wider public health goals by the pandemic — particularly in poorer nations. The World Health Organization said last month that, of the 11 countries with the highest malaria burden, only India registered progress against the disease in 2020, as testing and the distribution of treatments were hampered by the Covid crisis. The 10 other countries, all in Africa, reported increases in malaria cases and deaths, the WHO said.
The advent of other potentially life-saving Covid treatments, such as antivirals, could open up further inequalities, experts fear. In the global health community, the overriding concern is that a moment in history that could prompt nations to act jointly to forestall future public health emergencies must not be lost.
A report last year from the Global Preparedness Monitoring Board, a body co-convened by the World Health Organization and World Bank, blamed “geopolitical divisions” and a tendency for power brokers to negotiate behind closed doors without the people most affected for “multiple tragedies”. These ranged from “vaccine hoarding” to oxygen shortages in poor countries and “the shattering of fragile economies and health systems”.

Ingrid Katz, associate faculty director at research organisation the Harvard Global Health Institute, says that pandemics magnify inequalities in the global health system. She worries that, as attention on Covid starts to wane for many people over the next two years, “there will be less of an appetite to think about our global neighbours and how critical they are.”
As an example of the kind of international co-operation that can change the course of a disease outbreak, she cites the release of information by South African scientists on the sequencing of Omicron, This, she says, was “critical information and helped us at least have a knowledge of what was coming our way”.
Katz has been heartened by efforts in December by the World Health Assembly, the WHO’s decision-making body, to craft an international pandemic agreement. This, she says, will “define how we can address some of these gaps in global governance and the inequities that we saw play out in this pandemic”.
However, the coronavirus crisis has also exposed the shortcomings of individual countries’ health systems. Around the world, there is a growing awareness that, if healthcare systems are to prevent rather than simply cure disease, they must move beyond the silos that divide hospital care from primary and community care. They must now recognise the role played by institutions such as food banks in sustaining the poorest members of society.
This emphasis on prevention will involve greater focus on the social determinants of health — factors such as housing, food and the environment. Kieron Boyle, who heads Impact on Urban Health, a London-based healthcare organisation, identifies obesity and air pollution as the two biggest global concerns and says business will be under growing pressure to help address them.
Boyle anticipates that the pandemic’s “social backlog” will be felt strongly in 2022. He points out that people from deprived backgrounds have suffered disproportionately from illness and disrupted employment and education, and they now face the effects of rising inflation. “That’s going to bring another wave of health crises,” he warns.